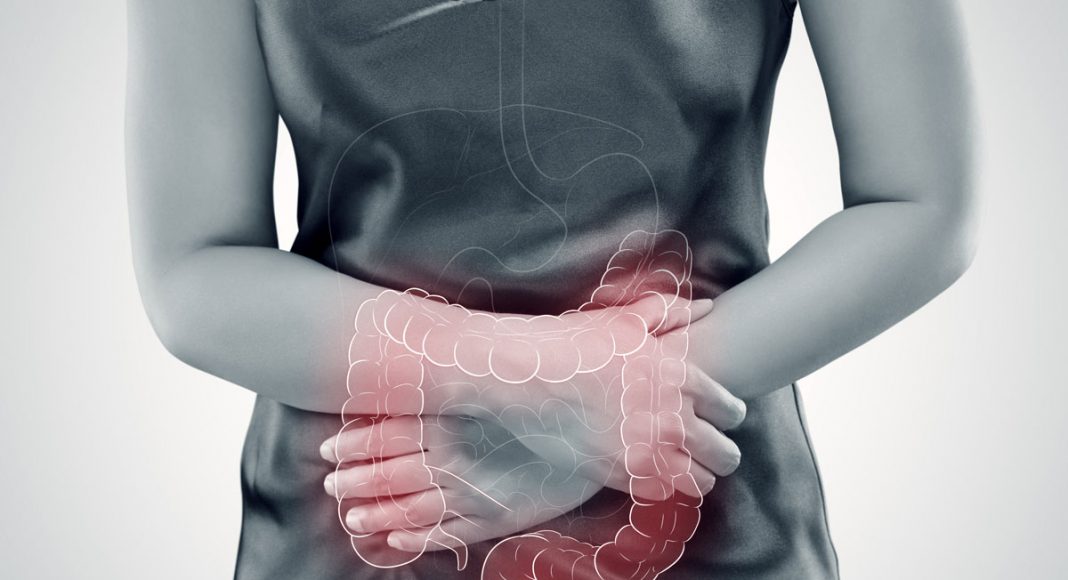
Because the endocannabinoid system acts as a regulatory system for your gut, it helps lower inflammation that would cause chronic issues.
A primary reason many patients turn to medicinal cannabis is to treat chronic pain. In fact, a 2019 study published in the journal Health Affairs found that more than 62% of medical marijuana patients were using the plant to relieve pain symptoms.
Those with chronic gut issues also experience intense pain, and patients with Inflammatory Bowel Disease (IBD), like Crohn’s and ulcerative colitis, have begun using medicinal cannabis to treat their symptoms. Though cannabis provides therapeutic value for these people, its primary benefit doesn’t really have to do with their pain.
Until recently, we weren’t exactly sure why cannabis was so effective in treating chronic gut problems. But a 2018 study published in the Journal of Clinical Investigation was able to show the physical manner in which cannabis attacks IBD. Researchers weren’t initially looking for marijuana’s effect on the microbiome, but rather stumbled upon the answer.
RELATED: The Impact Cannabis Has On Ulcerative Colitis
What cannabis was treating was their inflammation. Previous studies have shown how cannabis is a useful anti-inflammatory, but it works a little differently with IBD. First, a little anatomy lesson. A thin layer of cells, called epithelial cells, separates our gut from the rest of our bodies and are responsible for regulating different mechanisms, like controlling how many neutrophils enter.
Neutrophils are a kind of white blood cell that traverses the gut and eats up microbes. When too many neutrophils slip inside and kill peaceful microbes and the gut itself, it causes IBD in patients. But researchers discovered epithelial cells aren’t the only the gateway that controls what gets in our gut.
As Beth McCormick of the University of Massachusetts and others discovered, our endocannabinoid system also contributes. Think of the endocannabinoid system acting as a regulatory system for the gut. Not everyone produces enough cannabinoids to assist the gut in functioning properly, which helps explain why ingesting cannabinoids through cannabis has proven effective for patients.
“There’s been a lot of anecdotal evidence about the benefits of medical marijuana, but there hasn’t been a lot of science to back it up,” said McCormick, who served as co-author of the study.
“For the first time, we have an understanding of the molecules involved in the process and how endocannabinoids and cannabinoids control inflammation. This gives clinical researchers a new drug target to explore to treat patients that suffer from inflammatory bowel diseases, and perhaps other diseases, as well.”
RELATED: Cannabis And Gut Health: Does It Boost Your Gut Bacteria?
It’s worth mentioning that researchers have not conducted studies on using marijuana-derived cannabinoids to replace those missing in humans with IBD. But the team behind the study believes this could open the door to helping the 1.6 million Americans with IBD.
Randy Mrsny, a co-author of the study and professor at the University of Bath’s Department of Pharmacy and Pharmacology, said that “while this is a plausible explanation for why marijuana users have reported cannabis relieves symptoms of IBD, we have only worked in mice and have not proven this experimentally in humans.”
“However our results may provide a mechanistic explanation for anecdotal data that cannabinoid exposure benefits some colitis patients,” he added. “For the first time we have identified a counterbalance to the inflammation response in the intestine and we hope that these findings will help us develop new ways to treat bowel diseases.”