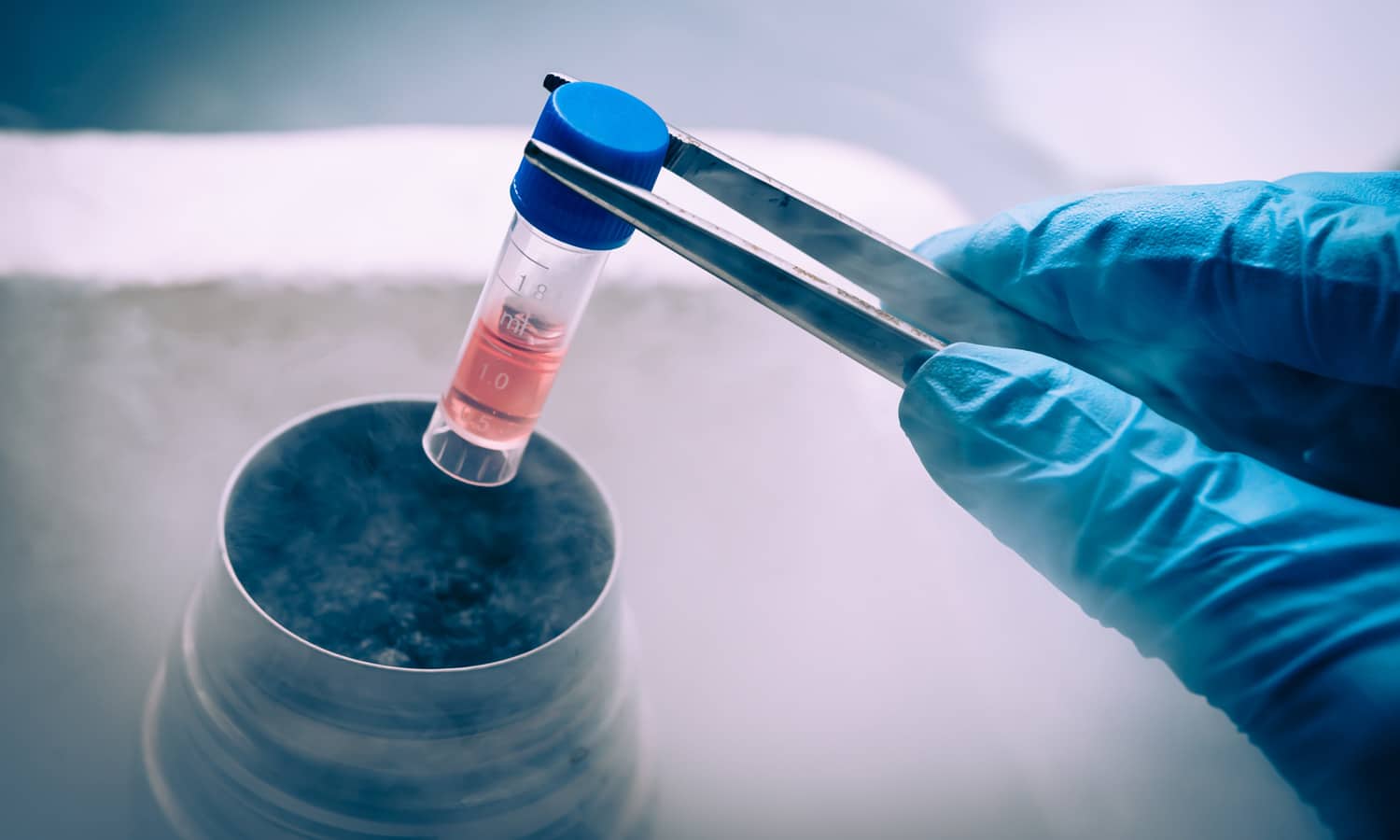
Those living with pulmonary fibrosis can develop other conditions, such as lung cancer, blood clots, pneumonia or high blood pressure.
Could stem cell secretions actually deliver a substance that can repair lung injuries for those with damage from pulmonary fibrosis? A recent study conducted at North Carolina State University examining a new form of inhalation therapy in rodents concludes that, “the work could lead to more effective, less invasive treatment for human pulmonary fibrosis sufferers.”
According to Mayo Clinic, pulmonary fibrosis is a disease that affects the lungs after tissue becomes damaged. The tissue becomes thicker, decreasing lung function and causing shortness of breath in many individuals.
Almost always fatal and non-curable, pulmonary fibrosis affects about 100,000 Americans today, according to the U.S. National Library of Medicine – Genetics Home Reference. Cited as a degenerative disease, or a condition that worsens over time, GHR also explained that those living with pulmonary fibrosis can develop other conditions, such as lung cancer, blood clots, pneumonia or high blood pressure:
“The course of the disease is highly variable; some affected people become seriously ill within a few months, while others may live with the disease for a decade or longer.”
This recent study, published in the journal Nature Communications, features the work of over a dozen researchers led by Ke Cheng, Professor of Regenerative Medicine at NCSU. Developing spheroid-produced lung stem cells (LSCs), the team was able to utilize the cells and test secretions through a “stem cell sauna,” or nebulizer treatment that allowed the mice and rats to inhale the therapy.
RELATED: Did Scientists Cure Type-1 Diabetes?
Knowing the therapeutic benefits of inhalation therapy, the team found that certain secretions from the stem cells had better benefits than others. These secretions, (LSC-Sec and LSC-Exo) showcased that the cells offered medicines which helped tissue to heal, easing inflammation.
“The mixture of cells in LSCs recreates the stem cells’ natural microenvironment — known as the stem cell niche — where cells secrete exosomes to communicate with each other just as they would inside your body,” says Cheng. “LSCs secrete many beneficial proteins and growth factors known collectively as ‘secretome’ — exosomes and soluble proteins which can reproduce the regenerative microenvironment of the cells themselves. In this work we took it one step further and tested the secretome and exosomes from our spheroid-produced stem cells against two models of pulmonary fibrosis.”
RELATED: Will Using Marijuana Reduce My Lung Capacity?
Looking to expand their testing to chronic obstructive pulmonary disease (COPD), acute respiratory distress syndrome (ARDS), and pulmonary hypertension (PH), the team is looking forward to researching how inhalation therapy can help ease disease in the lungs and perhaps offer a cure for those suffering with the many types of pulmonary fibrosis.
Co-author Kenneth Adler, Alumni Distinguished Graduate Professor at NC State, explained, “The finding that products released by lung stem cells can be just as efficacious, if not more so, than the stem cells themselves in treating pulmonary fibrosis can be a major finding that can have implications in many other diseases where stem cell therapy is being developed.”